Great Toe Mobility : The Linchpin to Movement Longevity | (Part 1 – Anatomy)
This past weekend I was fortunate to present at the Perform Better Summit in Providence, Rhode Island. This 3-day educational event is comprised of some of the best educators and most enthusiastic professionals in the industry. A common theme throughout a couple of the sessions was the association between great toe mobility and function.
The seemingly simple process of hallux dorsiflexion during push-off is actually quite complex and if great toe mobility is compromised it can cause a slew of movement compensations and pain patterns.
In this 3-part blog series we will begin to explore how this joint is stabilized, simple assessment techniques and programming which you can easily implement with your clients and athletes. Please note that these articles are not all-inclusive of every anatomical detail or compensation pattern – to learn more on this topic please check out our EBFA Certifications.
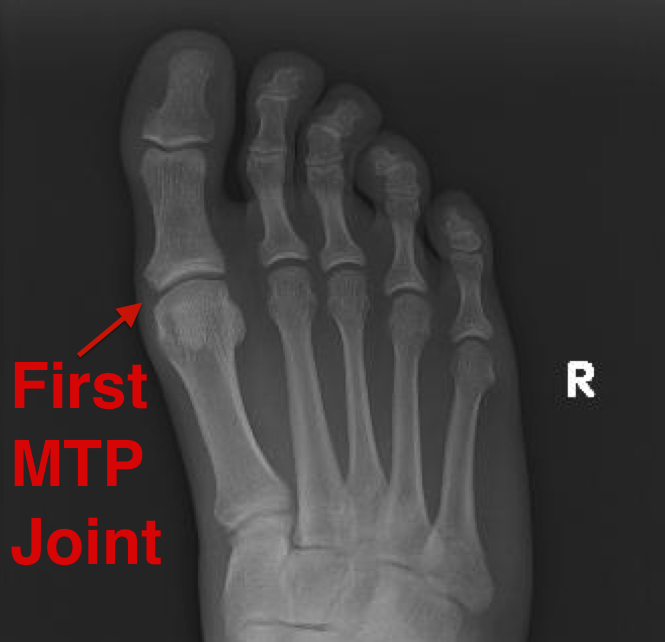 The 1st Metatarsophalangeal Joint (MPJ)
The 1st Metatarsophalangeal Joint (MPJ)
Formed by the head of the first metatarsal and base of the proximal phalanx this ginglymoarthrodial or hinge joint allows sagittal plane progression during walking, running, jumping etc.
With the movements of plantarflexion and dorsiflexion, optimal push-off during the gait cycle requires at least 30 degrees of dorsiflexion but having closer to 65 – 75 degrees dorsiflexion is ideal.
Limited hallux dorsiflexion during push-off can be associated with a low-gear push off position, early heel rise, overactive adductors and under active gluteus maximus.
Complexity of Hallux Dorsiflexion
At first glance 1st MPJ dorsiflexion seems quite straight forward and based on the increasing emphasis on the great toe in many fitness and performance lectures – I think it is imperative that professionals truly understand this joint and the complexity associated with hallux dorsiflexion. Improving hallux dorsiflexion requires much more than simply integrating great toe stretches or putting a wedge under the big toe.
So here we go. 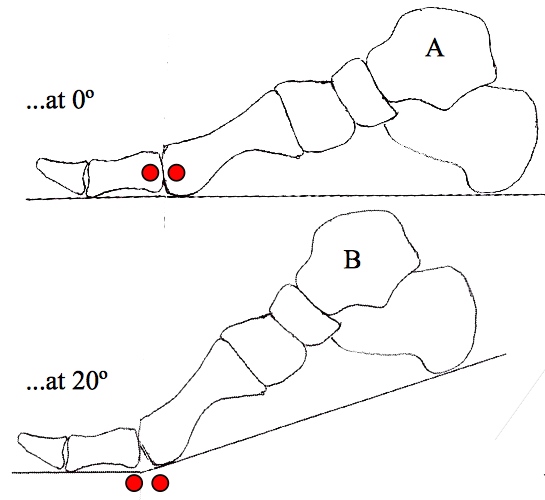
In closed chain movements such as walking, the propulsive phase of gait is the phase in which maximum great toe dorsiflexion is required. As the foot prepares for the large amount of power output during propulsion, the flexor hallucis longus (FHL) engages thereby anchoring the distal aspect of the hallux to the ground.
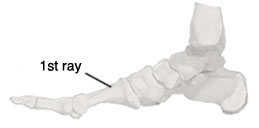
This fixed hallux provides a stable base or lever for propulsion thus allowing the metatarsal head to move relative to the base of the proximal phalynx. See picture to the right.
Sliding, Gliding and Jamming
If we break down hallux dorsiflexion even further will find that the first 20 degrees of dorsiflexion – the head of the 1st metatarsal slides over the base of the proximal phalanx.
The next 10 degrees – 50 degrees of dorsiflexion requires the 1st metatarsal to plantarflex relative to the base of the proximal phalynx creating a gliding movement as the foot moves over the hallux.
The final stage of hallux dorsiflexion is a jamming phase which holds the joint in a stable position.
To repeat – with each step we take – hallux push-off requires a timed movement pattern of sliding, gliding and jamming of the 1st metatarsal head relative to the base of the proximal phalanx. If the timing is shifted or the 1st metatarsal head cannot plantarflex relative to the proximal phalynx, then hallux dorsiflexion will be limited and compensation results.
So how do we ensure proper sliding, gliding and jamming?
1st ray stability!
Of the above phases the most important phase would be gliding phase or the plantarflexion of the 1st metatarsal head relative to the base of the proximal phalynx.
So then the question should be – how do we ensure that the 1st metatarsal head plantar flexes relative to the base of the proximal phalynx?
To answer this question we must know which muscle plantarflexes the 1st metatarsal.
For those who hav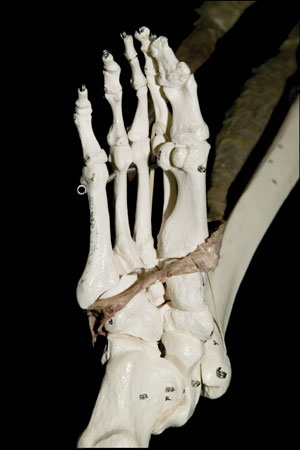 e taken my Barefoot Training Specialist courses – especially the Level 2 – you should recall that the muscle that plantarflexes the 1st metatarsal is the peroneus longus.
e taken my Barefoot Training Specialist courses – especially the Level 2 – you should recall that the muscle that plantarflexes the 1st metatarsal is the peroneus longus.
Running along the lateral aspect of the lower leg, behind the lateral malleolus and under the cuboid, this muscle attaches to the base of the 1st metatarsal and to the medial cuneiform.
If we look closer at the peroneus longus insertion we see that it inserts 90% on the base of the 1st metatarsal and only 10% on the medial cuneiform. Together this insertion controls the metatarso-cuneiform joint – or the 1st ray.
Joining the peroneus longus tendon on the medial side is the tibialis anterior, with both of these muscles together contributing to the Spiral Fascial Line.
1st Ray / Met-Cuneiform Stability
 With the tibialis anterior and peroneus longus as direct antagonists of each other, balance between these two muscles is critical for 1st ray stability or hallux dorsiflexion.
With the tibialis anterior and peroneus longus as direct antagonists of each other, balance between these two muscles is critical for 1st ray stability or hallux dorsiflexion.
If for some biomechanical or neuromuscular reason the tibialis anterior is more active or dominant compared to the peroneus longus then the 1st metatarsal (1st ray) begins to dorsflex. 
If the 1st metatarsal is dorsiflexed then the gliding phase of hallux dorsiflexion cannot occur and we get premature jamming of the 1st MPJ, limited dorsiflexion and compensation.
So how do we ensure balance between the tibialis anterior and peroneus longus?
To answer this question we must go to the rear foot where we will find the subtalar joint (STJ). STJ position greatly dictates
the stability of not just the rear foot, but the entire foot in general.
STJ eversion is often associated with a hyper mobile, flexible and unstable foot and often has trouble locking or stabilizing in a timely manne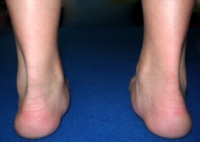 r. STJ eversion as indicted in the picture to the left also causes the peroneus longus tendon to go on slack thus giving a mechanical advantage to the tibialis anterior.
r. STJ eversion as indicted in the picture to the left also causes the peroneus longus tendon to go on slack thus giving a mechanical advantage to the tibialis anterior.
Once the tibialis anterior is given an advantage, the 1st metatarsal begins to dorsiflex, the stability of the 1st ray is compromised and hallux dorsiflexion is limited.
But what if you have a client with limited hallux dorsiflexion and they have a neutral STJ position? This is where understanding both open-chain and closed-chain assessment techniques is important.
In Part 2 of this blog series we will explore how to begin to assess for both structural and functional causes of limited hallux dorsiflexion.
Until then…..stay barefoot strong!
Dr Emily Splichal
Founder EBFA Fitness
